Getting Ready for the End of the Shift Nursing Freeze: Prior Authorization Packets
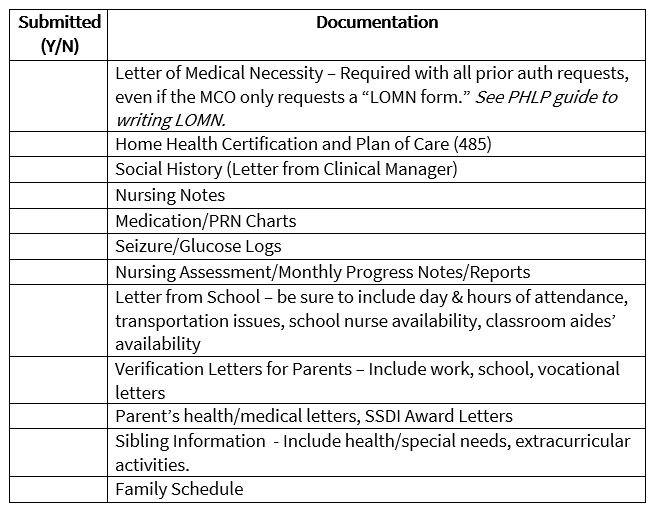
As previously reported, the freeze on prior authorization requirements for pediatric shift nursing care will lift on November 1, 2022. In preparation, it is critical to begin preparing a prior authorization packet for the number of shift nursing hours needed, even if your child’s Medicaid health plan has not asked for the packet yet. A strong prior authorization packet increases the chances that the Medicaid health plan approves the requested hours, thus avoiding the need for an appeal. Below you can find a prior authorization checklist to assist in obtaining the necessary documentation. You can also review PHLP’s guide to writing a letter of medical necessity.
Once the prior authorization packet is submitted, the Medicaid health plan has two (2) business days to notify you of the decision (i.e., whether the services are approved or denied), unless additional information is needed. If no additional information is needed, the Medicaid MCO must mail a written decision to you, your child’s PCP, and the prescribing provider. If current services are at issue, that notice must be sent at least 10 days in advance of the decision effective date. A phone call telling you or your home health agency about the decision does not negate the need for a written notice!
If additional information is needed to make the decision, the Medicaid health plan must request this information within 48 hours of receiving the prior authorization request, and must allow 14 days for submission of the additional information. If the requested additional information is not provided within 14 days, the Medicaid health plan must contact the prescribing provider at least once to confirm that all available documentation related to the requested nursing services has been submitted. Failure to provide the additional information requested will likely result in a denial.
If services are denied, you have the right to challenge that decision by filing an appeal. If you receive a denial of services your child is currently getting, request a grievance within 10 days to keep those services in place while the appeal is being decided. You can call PHLP for assistance for your appeal: 1-800-247-3258.