Medicaid Health Plan Changes: Take Action by August 16th
There are major changes coming to Pennsylvania’s Medicaid (or Medical Assistance) Physical HealthChoices Plans on September 1, 2022. The changes affect nearly 500,000 consumers who receive Medicaid coverage and who will need to choose a new health plan by August 16.
Who Is Impacted?
- Approximately 500,000 Medicaid enrollees must choose a new plan by August 16, 2022 because their current plan is going away. Other enrollees may change plans if they wish.
- Individuals in Community HealthChoices (CHC), the Children’s Health Insurance Program (CHIP), or in a Medicare Plan are not impacted.
- Between now and July 7, all impacted individuals will receive a mailing explaining the plan changes. These mailings will be sent to both those who must change plans and those who may change plans if they wish. The mailing will contain a letter explaining whether the consumer must change plans or simply may choose a new plan, a chart showing the plans that will be available in the consumer's zone beginning September 1, and instructions for how to change plans.
What Plans Are Changing?
Whether your plan choices are changing depends on where you live and which plan you are in. There are several major changes:
- Aetna will no longer operate a Medicaid plan anywhere in Pennsylvania after September 1. This does not affect Aetna's CHIP Plan, which will continue to operate as it has been.
- United will no longer operate in the Southwest and Lehigh/Capital zones. This does not affect United's CHIP plan, which will continue to operate as it has been.
- Highmark (formerly Gateway) will no longer operate in the Northwest zone. This does not affect Highmark's CHIP plan, which will continue to operate as it has been.
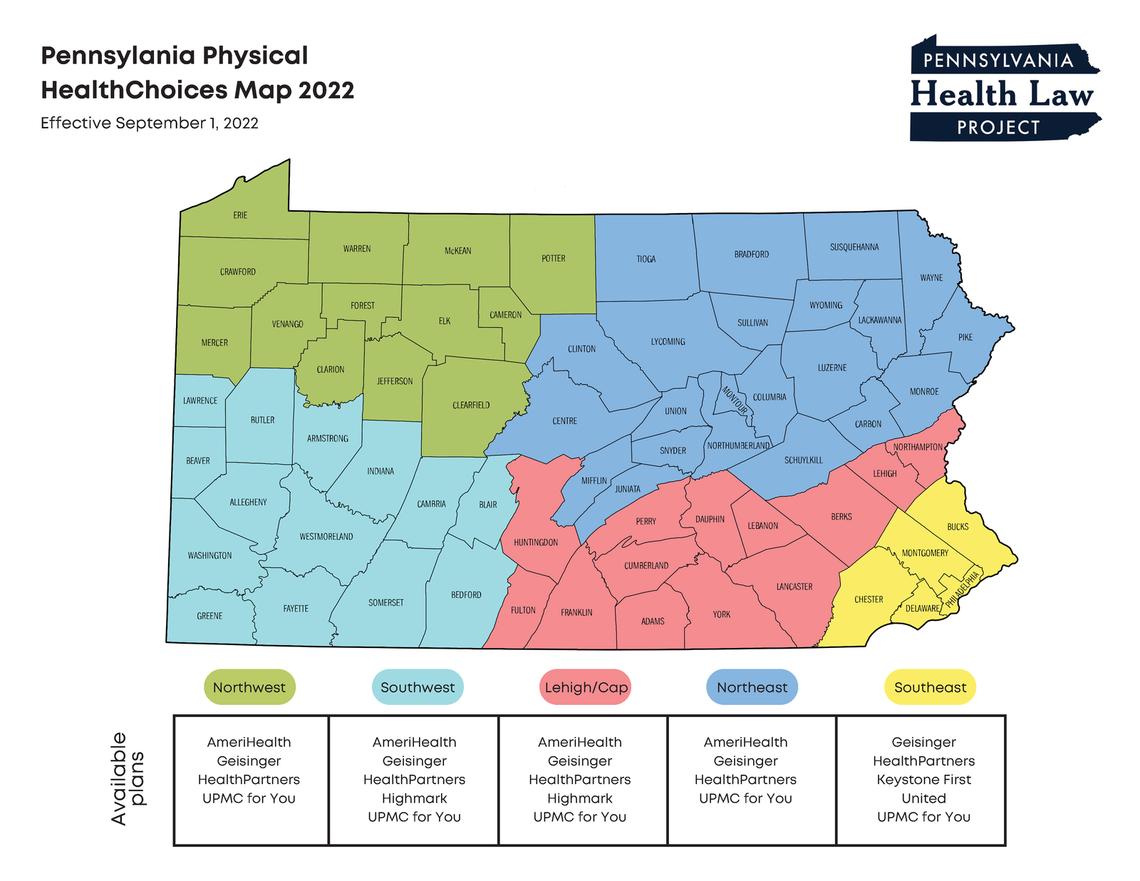
- New plans will be available in all zones across the state. To see the plans offered in your part of the state, see PHLP’s zone-by-zone breakdown.
What Do I Need to Do?
Enrollment has begun. Consumers must change plans by August 16. Consumers who are required to change plans, and do not change, will be auto-assigned to a new plan on August 17. To compare the available plans and to make a plan change, contact PA Enrollment Services online, on their app, or by phone:
- EnrollNow.Net: Enroll in a new plan through the enrollment service website, Enroll Now. Here, individuals can compare the health plans being offered in their respective regions and make the best decision. They can also find answers to frequently asked questions.
- Mobile app: Download the PA Enrollment Services mobile app (available free of charge through the Apple store or Google play).
- Phone: Call 1-800-440-3989 (TTY: 1-800-618-4225) and select Option 6 to speak with a representative. (Open Monday through Friday, 8 a.m. to 6 p.m.).
Where Can I Get More Information?
- The Department of Human Services (DHS) is holding virtual consumer meetings across the state. In these meetings, participants can discuss issues with enrollment and changing plans. A list of the meetings and their registration links can be found here.
- DHS has created a toolkit that discusses the plan changes and next steps for consumers. The toolkit can be found here.
- DHS has a website about the Medicaid plan changes, which is available here.
- PHLP created a factsheet to help consumers through the process of selecting a new plan. This resource gives consumers a step-by-step guide on what to consider when making their decision.
Consumers who have problems connecting online or by phone with PA Enrollment Services should call PHLP’s Helpline at 1-800-274-3258, Monday and Wednesday from 8 a.m. to 8 p.m.
